*A version of this story ran in USA Today *
I’m staring at black-and-white images of my brain.
“See this little white dot that almost looks like a star right there?” Diagnostic Radiologist Dr. Sean London asks over Zoom call. He’s sharing his screen with me while we go frame-by-frame over a high-tech, elective, full-body MRI scan I had a few weeks ago.
He points to a pencil-tip-sized grayish smudge on the right side, then uses his cursor to circle two more similar circles on the left. They look like specks of lint on top of an otherwise eerily vivid picture of … well … pretty much everything inside my skull.
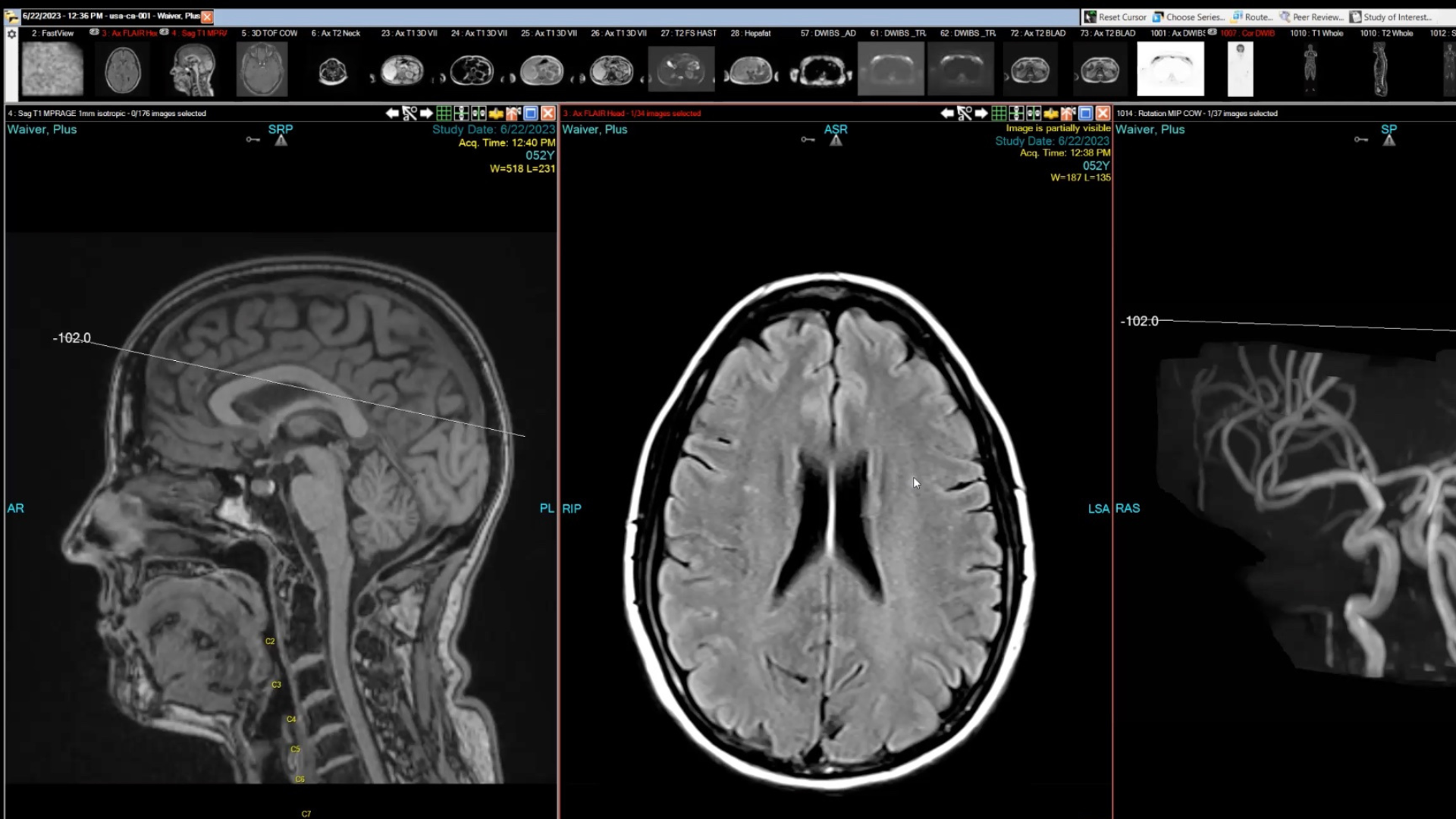
Screenshot of Jennifer Jolly’s Brain from the Prenuvo scan.
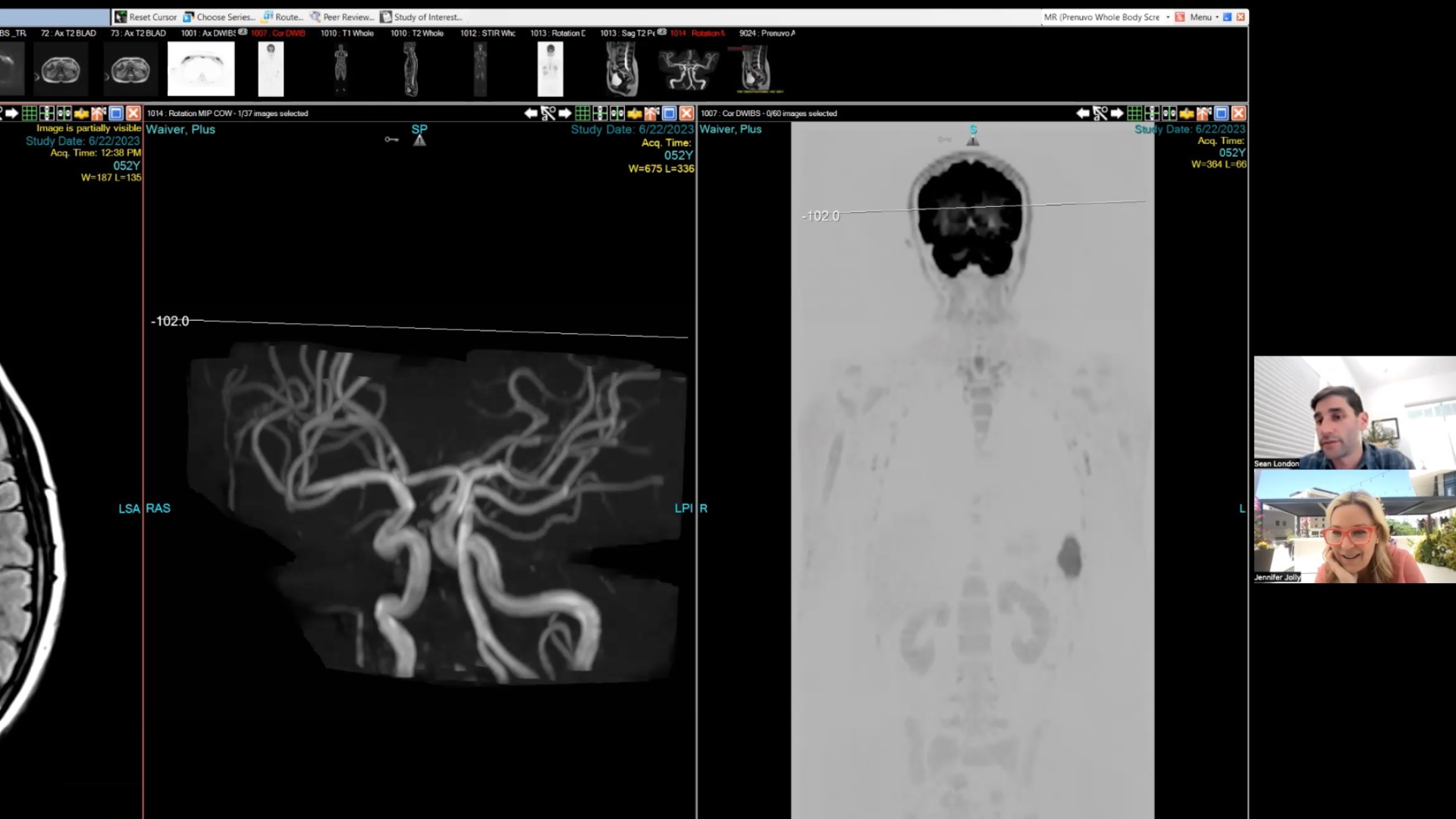
Screenshot of Jennifer and Dr. London going over her results.
“These are really common, and I’m not worried about them. I see these every single day.” Dr. London assures. “Sometimes they’re signs of migraines, or they can be from trauma where these small vessels get injured, and you can kind of think of them like scar tissue,” he pauses to see if I have any questions so far.
I tell him that I used to get horrible migraines and I’ve had several concussions.
“Well, we’ll keep an eye on them and make sure nothing changes. Your brain is healthy, and there’s no cause for concern,” he reiterates.
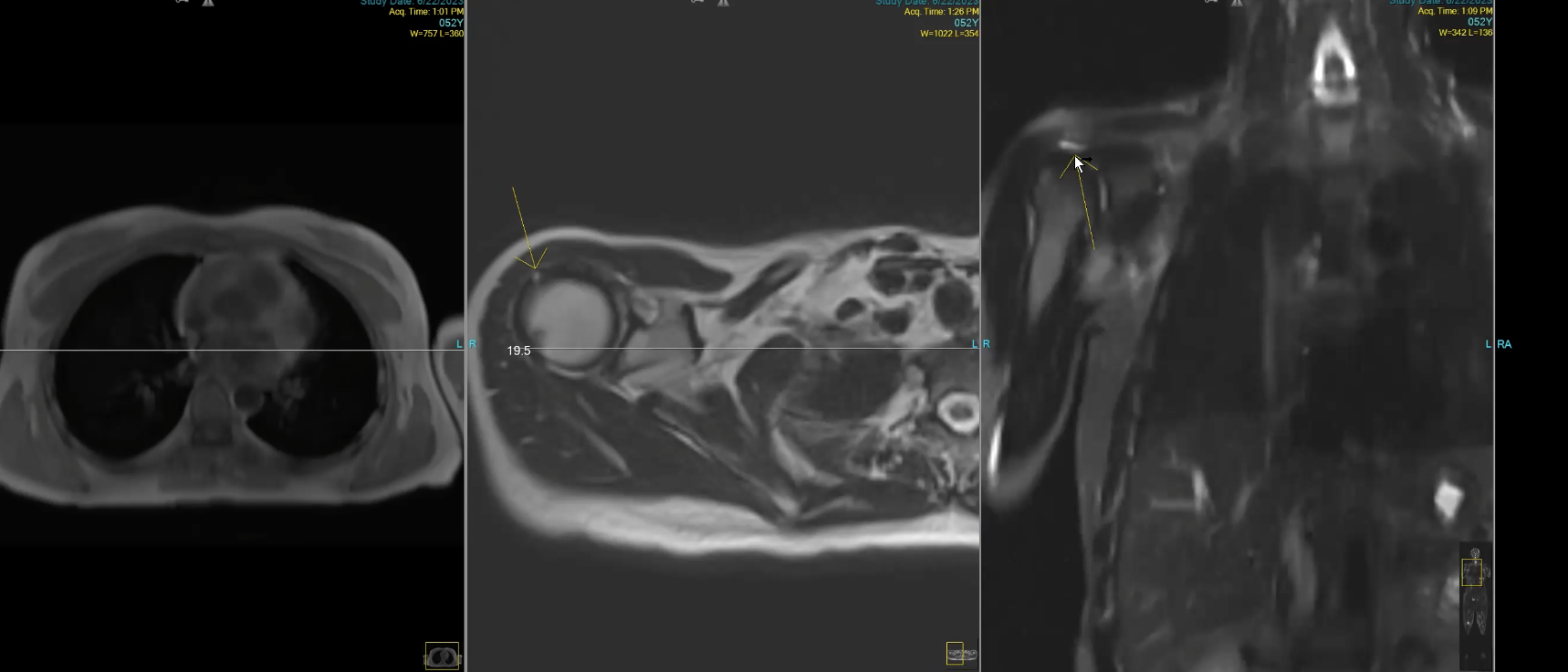
Dr. London points out a torn rotator cuff in Jennifer’s full-body MRI scan.
For the next 40 minutes, Dr. London takes me on a fascinating tour of the inside of my body, unlike anything I’ve ever experienced before.
I find out that the nagging pain in my right shoulder my primary care physician said was “a sign of age,” is a partially torn rotator cuff. (‘I knew it,’ I think. It happened when I fell off my horse several months ago, and it hasn’t worked the same since. Now I can do the right physical therapy and rehab it correctly.)
I also see a smattering of benign cysts; some I know about because I can feel them under my skin, and others, like one behind my left knee, are a complete surprise. None of this worries me, though. It’s a huge relief.
At 52, I’m strong, healthy, and aging better than ever. There are no signs of cancers, aneurysms, or degenerative diseases. Whew.
Several of my family members have not been so lucky.
WHY I DECIDED TO DO THE MRI.
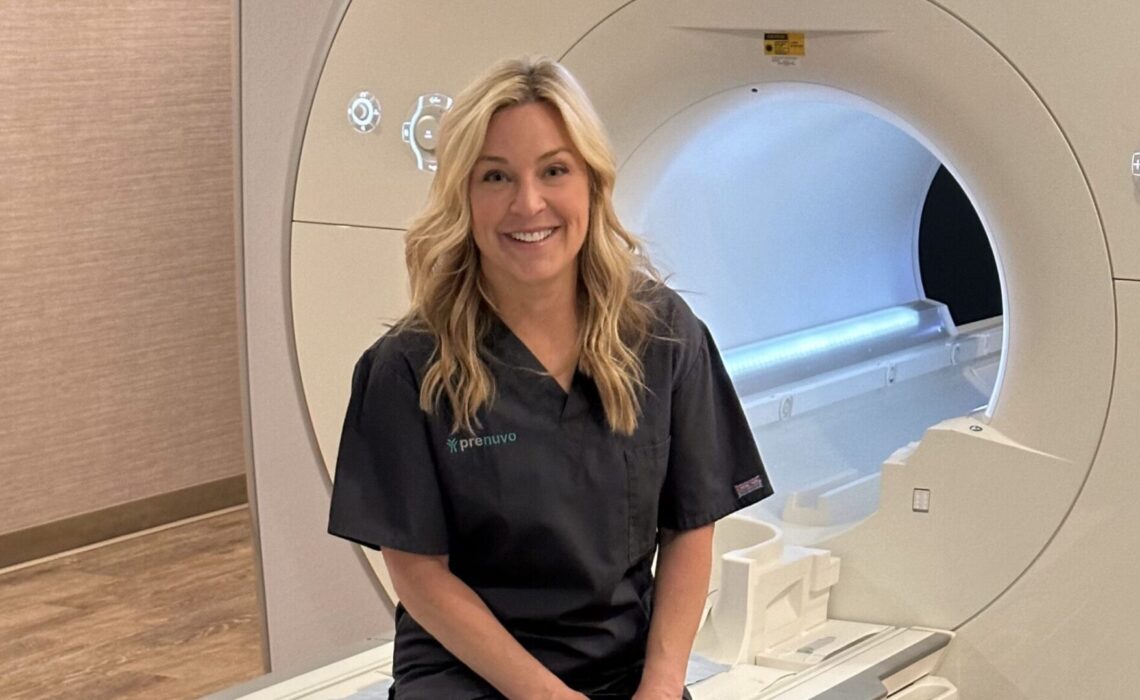
Jennifer Jolly is all smiles in advance of her Prenuvo scan.
I’m adopted, so genetic medical information has, for the most part, been a massive mystery. But I met my birth mother as an adult, and she was sick. She died a few years ago from lung damage caused by a genetic condition called Alpha-1 antitrypsin deficiency.
Then, about a year and a half ago, I met my half-sisters on my birth father’s side. One of them has been in remission from breast cancer for 20 years. It came back this summer, and updated DNA tests show it’s hereditary.
She’s currently in her third battle against an aggressive disease that’s infected her lymph nodes and potentially spread to other parts of her body. In the last two months, she’s had major surgery and is now in the middle of chemotherapy, with months of radiation to follow.
Not long after she called to tell me about her diagnosis, I found a lump.
When I mentioned all of this at my 10-minute-long annual visit with my primary care physician, she said we could revisit it all next year if I started showing any symptoms.
I didn’t love that answer. As I’ve reported before, my monthly bill for health insurance is $825 (I’m self-employed), yet that was only my second checkup in four years. That math works out to nearly $20,000 for that ten-minute appointment.
If an hour-long, non-invasive, safe, full-body MRI scan could give me something even remotely close to a crystal ball look into my health in an empowering versus alarming way, why on earth would I not do it?
MONEY. It’s a huge cost for the average American, and insurance doesn’t cover it.
EARLY DETECTION OR WASTE OF RESOURCES?
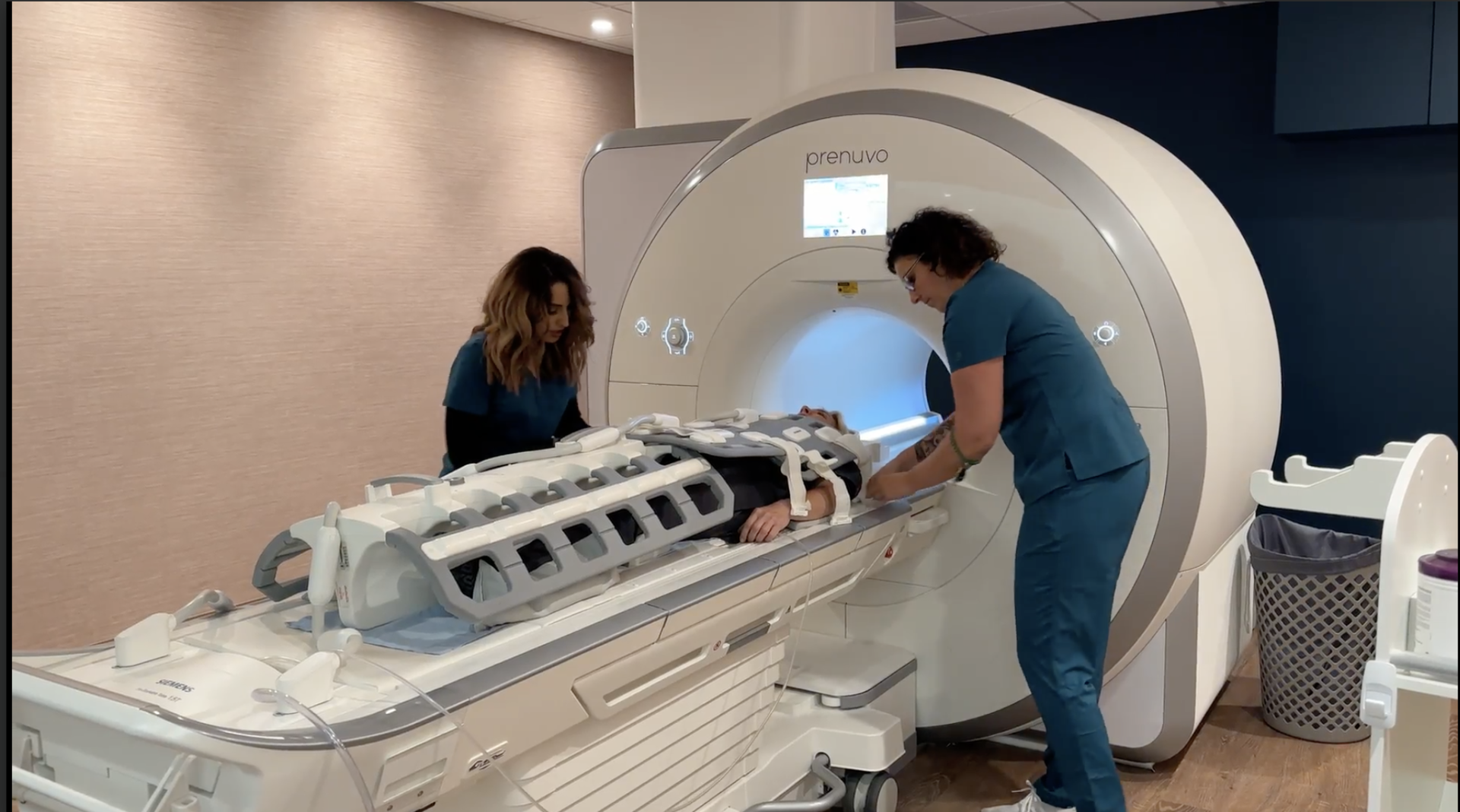
Jennifer Jolly getting strapped into the Prenuvo MRI scanner.
I did my scan at Prenuvo in Redwood City, California — right in the heart of Silicon Valley. It’s one of eight current Prenuvo sites operating around the United States and Canada, with 12 more opening over the next year.
The clinic is like many other spotless spa-like diagnostic centers in an area where the median cost of a home is edging close to three million dollars. Scans here start at $1,000. The out-of-pocket cost for the full body scan I had was $2,500.
Prenuvo says the full-body MRI scan screens for 500 conditions, including most tumors, aneurysms, and cysts. They also say their MRIs show potentially life-saving insights for one out of every 20 people they see. That includes actress and TV host Maria Menounos’. She credits Prenuvo with finding her Stage 2 pancreatic cancer after doctors told her the abdominal pain she was having was “nothing.”
“Basically what this is, is a physical exam, but taking pictures of the inside, so it’s just getting a direct insight into your body’s health,” Dr. London tells me during a sit-down interview after my scan. “We talk a lot about preventative care, but we don’t see a lot of action. I think this is one way to really contribute towards the whole of preventative care that people are looking for.”
A series of professionally shot video testimonials on YouTube underscore this point. There’s a 47-year-old Army vet discovering a Stage 3 tumor in his kidney and a mother of two finding out she has thyroid cancer.
Feedback from everyone I’ve spoken with who has had a Prenuvo scan, including my own husband, is overwhelmingly positive. The scan turned up a “shadow” on his pancreas that his primary care team will now monitor too.
NOT EVERYONE IS A FAN OF FULL-BODY MRI SCANS.
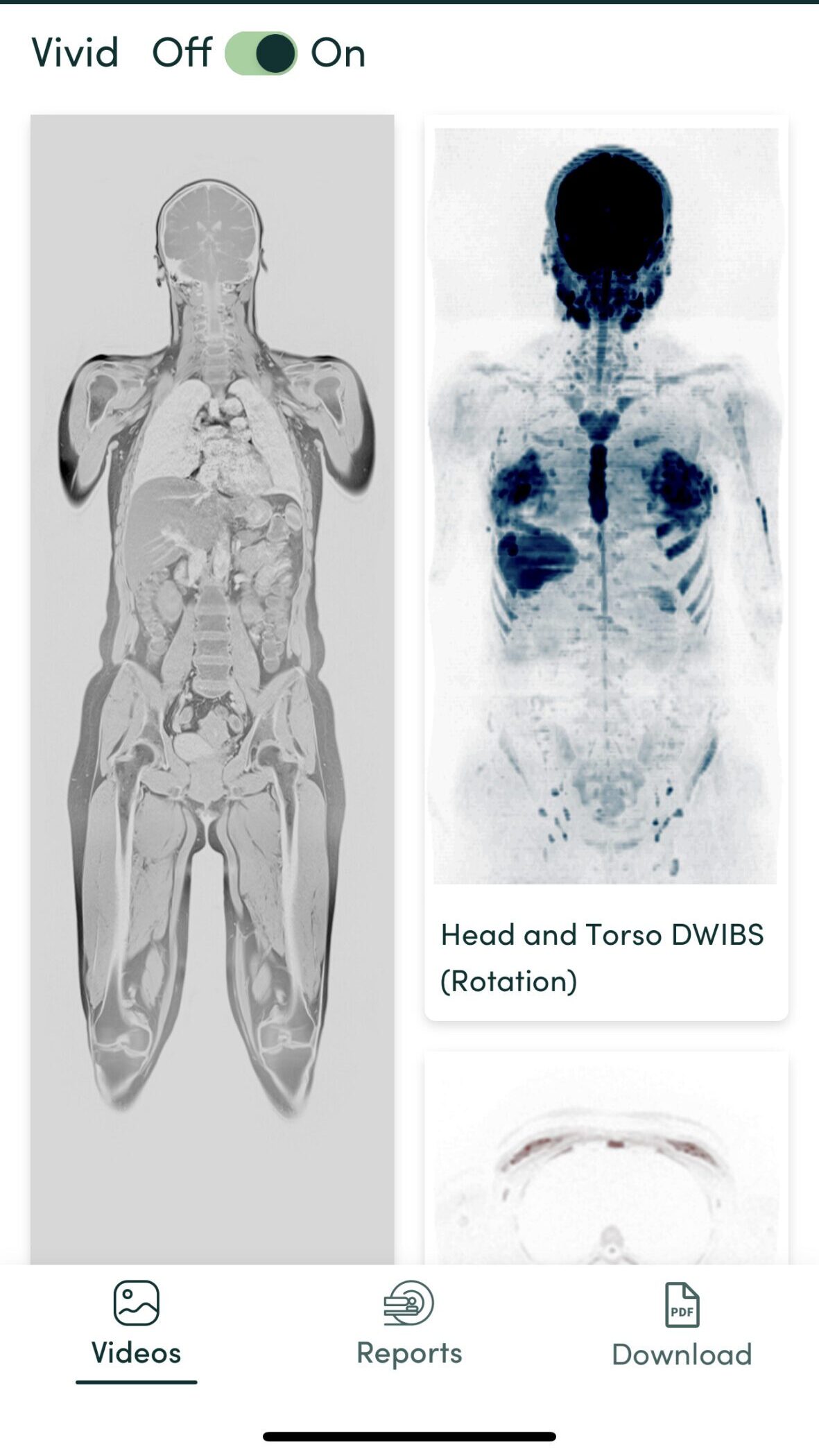
Videos of Jennifer’s scan on the Prenuvo app.
You know who doesn’t like them? Many family doctors, radiologists, and specialists who say they often cause more problems than they solve.
“The ‘incidentaloma’ is an exponentially growing entity, as more people get imaging that is unnecessary and unwarranted,” renowned spinal surgeon and CMO of Sword Health, Dr. Vijay Yanamadala tells me via email. “It is not only a significant cost to the system, but it also creates significant psychological distress for individuals who now have to deal with potentially months of work-up to conclude that it was an incidental finding. I see this all the time in my patients.”
The American College of Preventive Medicine recommends against full-body MRI scans in people who don’t have any red-flag symptoms. The American College of Radiology also released a statement earlier this year saying that there’s no “documented evidence that total body screening is cost-efficient or effective in prolonging life.”
Board-certified spine surgeon, Dr. Rahul Shah, adds that the lack of standardization in boutique clinics could be a concern as well.
“Unlike established screening tools like mammograms or colonoscopies, there is no standardized protocol for full-body MRI scans in asymptomatic individuals,” Dr. Shah wrote in an email. “This lack of standardization can lead to variability in results and recommendations … leading to unnecessary worry, additional testing, and potential harm.”
IS A PRENUVO SCAN WORTH IT?

Dr. Sean London going over scan results.
Full-body preventative MRI scans are more common in other countries, such as Taiwan, where initial studies show a correlation between “improved clinical outcomes, including greater life expectancy and reduced mortality rates.” The study, published in the National Library of Medicine, says it needs further research to establish a direct link.
This kind of scan wouldn’t work for a hypochondriac or someone who isn’t able to hear the intricacies of the findings. Dr. London was incredibly good with both me and my husband in explaining what he found and what level, if any, follow-up we should do as a result. This experience alleviated stress and worry, not the other way around. There were zero downsides for us or our primary care providers.
THERE HAS TO BE MORE THAN EATING HEALTHY AND EXERCISING…
Technology is an amazing tool for personal safety and health. We have written in the past about so many apps and gadgets that can do things like alert your doctor or 911 when you fall, crash, or even if you are having a heart event.
But, when it comes to proactive versus reactive healthcare, there has to be more modern medicine can do than tell us to exercise and eat right. Especially given that four in ten people will develop cancer in their lifetime, and studies show women are diagnosed later than men in more than 700 diseases.
I cannot tell you how many times I’ve ignored or downplayed my own symptoms until I have the worst case of whatever-it-is the doctor has ever seen. Now, for the first time in my life, I have a baseline to assess my health beyond how I feel on any given day.
While this might not save my life right now, it may very well in the future.
“Medicine, as innovative as it is, can take time to move forward,” Dr. London says carefully when we talk about these concerns. “We don’t really practice wellness,” he adds. “We’re trying to change that.”
Jennifer Jolly is an Emmy Award-winning consumer tech columnist and on-air correspondent. Read Jennifer’s latest columns at USAToday.com/tech or follow her @JennJolly on Instagram.
